Global Health Awareness 2026: Why It Matters More Than Ever
The Rising Importance of Health Unity Across Nations
World Health Day 2026 revolves around a simple yet powerful idea—we are all connected, whether we like it or not. Diseases don’t respect borders, climate issues don’t stop at checkpoints, and health inequalities ripple across continents. That’s exactly why global health awareness 2026 is gaining so much attention. It’s no longer just about individual well-being or even national healthcare systems; it’s about recognizing that the health of one region can directly impact the rest of the world.
Think about it like a domino effect. A virus emerging in a remote region can, within weeks, disrupt economies, overwhelm hospitals, and change daily life across the globe. We’ve seen this happen before, and the lesson is clear—health unity is not optional anymore; it’s essential. Governments, organizations, and communities are increasingly realizing that collaboration is the only way forward.
What makes this year different is the emphasis on “One World, One Health, One Science.” It’s not just a slogan—it’s a mindset shift. Instead of fragmented approaches, there’s a growing push toward unified strategies that consider multiple factors at once. The idea is to stop reacting to crises and start preventing them through shared knowledge and resources.
At the heart of this movement is awareness. When people understand how interconnected health systems are, they become more proactive—whether it’s supporting vaccination programs, advocating for clean environments, or simply staying informed. Global health awareness 2026 is about empowering individuals while strengthening collective responsibility, making health a truly global mission rather than a localized concern.

Key Challenges Driving Global Health Awareness Today
Despite progress, several challenges continue to push global health awareness 2026 into the spotlight. One of the biggest is inequality. While some countries have cutting-edge healthcare systems, others struggle with basic access to clean water and medical supplies. This imbalance doesn’t just affect those regions—it creates vulnerabilities that can spread globally.
Another major issue is the rise of emerging infectious diseases. Many of these diseases originate from animals or environmental disruptions, making them harder to predict and control. Add to that increasing urbanization, deforestation, and climate change, and you’ve got a perfect storm for new health threats. These factors highlight the urgent need for a more integrated healthcare approach, which we’ll explore next.
There’s also the challenge of misinformation. In today’s digital age, false health information can spread faster than viruses themselves. This complicates public health efforts and undermines trust in science. Combating this requires not just better communication but also stronger collaboration between scientists, governments, and media platforms.
Economic pressures also play a role. Many countries face budget constraints that limit healthcare investments, especially in preventive measures. Ironically, neglecting prevention often leads to higher costs in the long run, particularly during outbreaks or health crises.
All these challenges point to one conclusion: isolated efforts are no longer enough. Addressing global health issues requires coordinated, science-driven strategies that bring together multiple sectors. The growing awareness around these challenges is what’s driving the momentum behind World Health Day 2026, pushing the world toward a more unified and proactive health system.
Understanding the Integrated Healthcare Approach
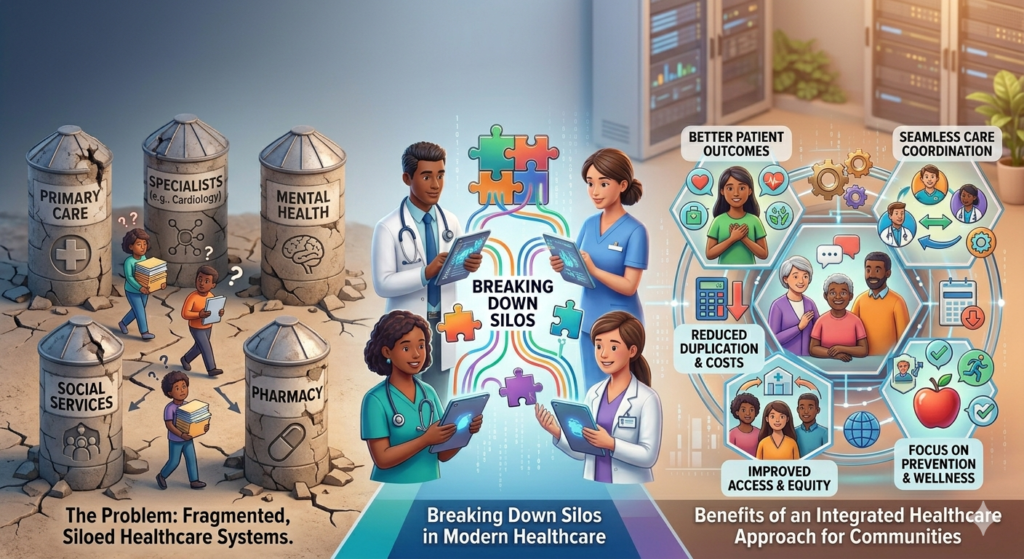
Breaking Down Silos in Modern Healthcare Systems
The traditional healthcare model has long operated in silos—hospitals focus on treatment, environmental agencies handle ecological concerns, and veterinary services deal with animal health. While each plays a vital role, this fragmented system often leads to missed connections. That’s where the integrated healthcare approach comes in, reshaping how we think about health as a whole.
Instead of viewing health through isolated lenses, this approach brings everything together. Imagine a system where doctors, environmental scientists, and veterinarians collaborate in real time, sharing data and insights. It sounds idealistic, but it’s increasingly becoming a reality. And honestly, it makes perfect sense—after all, how can we fully understand human health without considering the environment we live in or the animals we interact with?
One of the biggest advantages of this approach is early detection. For instance, if veterinarians notice unusual patterns in animal illnesses, it could signal a potential risk to humans. By sharing this information across sectors, preventive measures can be taken before a disease spreads widely. This is particularly crucial for managing zoonotic diseases, which account for a significant portion of emerging infections.
Another key aspect is efficiency. Integrated systems reduce duplication of efforts and allow for better resource allocation. Instead of multiple agencies working independently, they collaborate toward a common goal, making the entire system more effective.
Of course, breaking down silos isn’t easy. It requires changes in policy, infrastructure, and mindset. But the benefits far outweigh the challenges. As the world becomes more interconnected, the integrated healthcare approach is not just an innovation—it’s a necessity for building resilient health systems.
Benefits of an Integrated Healthcare Approach for Communities
When you zoom in from a global perspective to a community level, the impact of an integrated healthcare approach becomes even more tangible. It’s not just about big policies or international collaborations—it’s about improving everyday lives in practical, meaningful ways.
For starters, communities benefit from more comprehensive care. Instead of addressing symptoms in isolation, healthcare providers can consider a wider range of factors, including environmental conditions and lifestyle influences. This leads to more accurate diagnoses and effective treatments. It’s like solving a puzzle where every piece finally fits together.
Prevention is another major advantage. Integrated systems emphasize proactive measures, such as vaccination programs, environmental monitoring, and public education. These efforts reduce the likelihood of outbreaks and chronic health issues, ultimately saving lives and resources.
There’s also a strong economic benefit. Healthier communities mean lower healthcare costs and higher productivity. When people are well, they can work, learn, and contribute to society more effectively. This creates a positive cycle that supports both individual well-being and economic growth.
Perhaps one of the most underrated benefits is trust. When communities see different sectors working together seamlessly, it builds confidence in the system. People are more likely to follow health guidelines and participate in initiatives when they feel that the system is coordinated and transparent.
In essence, the integrated healthcare approach transforms healthcare from a reactive system into a proactive one. It shifts the focus from treating illness to maintaining wellness, aligning perfectly with the broader goals of World Health Day 2026. And as more communities adopt this model, the vision of “One World, One Health, One Science” becomes increasingly achievable.
Human Animal Environmental Health: The Core of One Health

How Human, Animal, and Environmental Health Interconnect
If you strip the idea of health down to its roots, you’ll notice something fascinating—nothing exists in isolation. Humans depend on animals for food, companionship, and even economic survival. At the same time, both humans and animals rely heavily on the environment for clean air, water, and resources. This intricate web is what defines human animal environmental health, the foundation of the One Health initiative.
Picture it like a triangle where each side supports the others. If one side weakens, the entire structure becomes unstable. For instance, environmental degradation—like deforestation or pollution—doesn’t just harm ecosystems. It forces wildlife into closer contact with humans, increasing the risk of disease transmission. Suddenly, what seemed like an environmental issue becomes a public health crisis.
Another example lies in food systems. Livestock health directly impacts human nutrition and safety. If animals are exposed to contaminated environments or poor conditions, it can lead to unsafe food supplies and the spread of diseases. This connection reinforces why monitoring animal health is just as important as human healthcare.
Climate change also plays a significant role here. Rising temperatures and shifting weather patterns are altering habitats, affecting both wildlife and human populations. Diseases that were once confined to certain regions are now spreading to new areas, challenging traditional healthcare systems. This dynamic clearly shows how environmental health impact is deeply intertwined with human well-being.
Understanding these connections isn’t just academic—it’s practical. By addressing health issues through this interconnected lens, we can identify risks earlier and respond more effectively. The One Health initiative thrives on this principle, encouraging collaboration across disciplines to create solutions that benefit all three domains simultaneously.
Real-World Examples of Human Animal Environmental Health Impact
It’s one thing to talk about theory, but real-world examples make human animal environmental health come alive. Take the case of avian influenza, often known as bird flu. This disease originates in birds but has the potential to infect humans, especially in areas where people live in close proximity to poultry. Here, animal health, human health, and environmental conditions all intersect in a very real way.
Another striking example is antimicrobial resistance (AMR). Overuse of antibiotics in both humans and animals has led to bacteria that no longer respond to treatments. This isn’t just a medical issue—it’s an environmental one too, as these resistant bacteria can spread through water systems and soil. Addressing AMR requires coordinated efforts across healthcare, agriculture, and environmental management.
Then there’s the issue of water contamination. In many parts of the world, industrial waste and agricultural runoff pollute water sources. This affects not only human populations but also aquatic life and ecosystems. Contaminated water can lead to outbreaks of diseases like cholera, illustrating how environmental neglect directly impacts public health.
Even urbanization plays a role. As cities expand, natural habitats shrink, bringing humans and wildlife into closer contact. This increases the chances of zoonotic diseases—illnesses that jump from animals to humans. It’s a vivid reminder that development without sustainability can have unintended health consequences.
These examples highlight a simple truth: health challenges are rarely confined to a single domain. They ripple across systems, affecting multiple aspects of life. Recognizing this interconnectedness is key to designing effective interventions and building a healthier, more resilient world.
Public Health Collaboration in a Connected World

The Role of Governments, NGOs, and Private Sectors
No single entity can tackle global health challenges alone. That’s where public health collaboration comes into play, acting as the glue that binds various stakeholders together. Governments, non-governmental organizations (NGOs), and the private sector each bring unique strengths to the table, and when they work in harmony, the results can be transformative.
Governments often set the stage by creating policies, funding healthcare systems, and coordinating national responses. They have the authority to implement large-scale programs, such as vaccination drives or disease surveillance systems. However, their efforts are significantly enhanced when supported by NGOs, which often operate at the grassroots level and have a deep understanding of local communities.
The private sector, on the other hand, drives innovation. Pharmaceutical companies develop vaccines and treatments, while tech firms create tools for data analysis and communication. When these innovations are aligned with public health goals, they can accelerate progress in ways that traditional systems alone cannot achieve.
A great example of successful public health collaboration is the global response to pandemics. International organizations like the World Health Organization (WHO) coordinate efforts across countries, ensuring that information, resources, and strategies are shared effectively. This kind of cooperation is essential for managing health crises that don’t respect borders.
What makes collaboration truly effective is trust and transparency. When stakeholders communicate openly and align their objectives, they can overcome challenges more efficiently. It’s not always easy—differences in priorities and resources can create friction—but the benefits far outweigh the obstacles.
Technology as a Catalyst for Public Health Collaboration
Technology has become a game-changer in public health collaboration, acting as a bridge that connects people, data, and ideas across the globe. From real-time disease tracking to telemedicine, digital tools are transforming how we approach health challenges.
One of the most impactful innovations is data sharing. Advanced analytics and artificial intelligence allow researchers to identify patterns and predict outbreaks before they escalate. This proactive approach is crucial for global disease prevention, enabling quicker and more targeted responses.
Telemedicine is another powerful tool. It breaks down geographical barriers, allowing patients in remote areas to access healthcare services without traveling long distances. This not only improves access but also reduces the burden on healthcare facilities, making systems more efficient.
Mobile technology also plays a significant role. Health apps and messaging platforms are used to disseminate information, track symptoms, and even monitor treatment adherence. During health crises, these tools become lifelines, keeping people informed and connected.
Blockchain technology is emerging as a solution for secure data sharing, ensuring that sensitive health information is protected while still being accessible to authorized parties. This is particularly important for international collaborations where data privacy concerns can be a barrier.
In essence, technology amplifies the impact of collaboration. It enables faster communication, better decision-making, and more effective interventions. As we move forward, integrating technology into public health strategies will be essential for achieving the goals of World Health Day 2026.
Building Sustainable Health Systems for the Future

Key Elements of Sustainable Health Systems
Creating sustainable health systems isn’t just about maintaining hospitals or funding healthcare programs—it’s about building systems that can withstand challenges, adapt to change, and continue to serve populations effectively over time. In the context of global health awareness 2026, sustainability has become a central theme, reflecting the need for long-term solutions rather than short-term fixes.
One of the core elements of sustainability is accessibility. Healthcare services must be available to everyone, regardless of location or socioeconomic status. This ties directly into the concept of health equity worldwide, ensuring that no one is left behind. Accessibility isn’t just about physical infrastructure; it also includes affordability and cultural relevance.
Another crucial component is workforce development. Healthcare systems rely heavily on skilled professionals, from doctors and nurses to community health workers. Investing in education, training, and retention is essential for maintaining a strong workforce capable of addressing diverse health challenges.
Resource management also plays a significant role. Sustainable systems use resources efficiently, minimizing waste and maximizing impact. This includes everything from medical supplies to energy consumption in healthcare facilities. Incorporating renewable energy and eco-friendly practices can further enhance sustainability.
Data-driven decision-making is another key element. By leveraging technology and analytics, healthcare systems can identify trends, allocate resources more effectively, and improve outcomes. This aligns closely with the goals of the One Health initiative, which emphasizes evidence-based approaches.
Ultimately, sustainable health systems are those that can evolve. They are resilient, adaptable, and inclusive, capable of meeting current needs while preparing for future challenges.
Challenges in Achieving Sustainability in Healthcare
While the vision of sustainable health systems is compelling, achieving it is far from straightforward. One of the biggest hurdles is funding. Many countries struggle to allocate sufficient resources to healthcare, especially when faced with competing priorities like education and infrastructure.
Another challenge is inequality. Disparities in wealth and resources mean that some regions can invest heavily in healthcare, while others lag behind. This creates gaps that undermine global health efforts and make global disease prevention more difficult.
Political instability can also disrupt healthcare systems, affecting everything from funding to service delivery. In such environments, maintaining consistency and long-term planning becomes a significant challenge.
Technological disparities further complicate the picture. While some countries benefit from advanced healthcare technologies, others lack basic digital infrastructure. Bridging this gap is essential for ensuring that innovations reach those who need them most.
Finally, there’s the issue of cultural and behavioral factors. Health practices and beliefs vary widely across populations, and implementing standardized solutions can sometimes lead to resistance. Addressing these challenges requires culturally sensitive approaches and strong community engagement.
Despite these obstacles, progress is possible. By fostering collaboration, investing in innovation, and prioritizing equity, the world can move closer to building health systems that are truly sustainable.
Global Disease Prevention Through One Health Initiative

Strategies for Effective Global Disease Prevention
When it comes to safeguarding humanity, global disease prevention is the ultimate goal—and the One Health initiative is one of the smartest ways to get there. Instead of reacting to outbreaks after they spiral out of control, this approach focuses on stopping diseases before they even begin. Sounds ideal, right? But in practice, it requires a deep level of coordination, foresight, and commitment across multiple sectors.
One of the most effective strategies is early surveillance. By monitoring human populations, animal health, and environmental conditions simultaneously, health experts can identify warning signs long before a crisis unfolds. Think of it like a smoke detector for global health—it alerts you before the fire spreads. This proactive system is especially important for detecting zoonotic diseases, which often originate in animals before jumping to humans.
Vaccination programs also play a huge role in global disease prevention. When implemented effectively, they not only protect individuals but also create herd immunity, reducing the overall spread of diseases. However, for these programs to succeed, they must be accessible and widely accepted, which ties back to public health collaboration and community trust.
Another critical strategy is education. People need to understand how diseases spread and what they can do to protect themselves. Simple practices like proper hygiene, safe food handling, and responsible antibiotic use can make a significant difference. Education empowers individuals to become active participants in disease prevention rather than passive recipients of care.
Environmental management is equally important. Reducing pollution, protecting natural habitats, and ensuring clean water supplies all contribute to better health outcomes. These measures address the root causes of many health issues, making them essential components of the One Health initiative.
Ultimately, effective prevention is about thinking ahead. It’s about connecting the dots between different sectors and acting before problems escalate. With the right strategies in place, the vision of a healthier, safer world becomes much more attainable.
Case Studies of Successful One Health Initiative Programs
Real-world success stories bring the One Health initiative to life, showing how theory can translate into tangible results. One notable example is the global effort to combat rabies. Through coordinated vaccination campaigns targeting both humans and dogs, several countries have significantly reduced rabies cases. This approach highlights the importance of addressing animal health to protect human populations.
Another compelling case is the response to the Ebola outbreaks in West Africa. By integrating human healthcare with wildlife monitoring and environmental management, health organizations were able to identify transmission patterns and implement targeted interventions. This collaborative approach not only contained the outbreak but also improved preparedness for future incidents.
The fight against avian influenza also demonstrates the power of global disease prevention through collaboration. Governments, international organizations, and the poultry industry worked together to monitor bird populations, implement biosecurity measures, and develop vaccines. These efforts helped prevent widespread transmission and minimized economic losses.
In Southeast Asia, integrated programs addressing antimicrobial resistance have shown promising results. By regulating antibiotic use in both healthcare and agriculture, these initiatives have slowed the spread of resistant bacteria. This is a perfect example of how healthcare innovation science can be applied across sectors to tackle complex challenges.
These case studies share a common thread: collaboration. They show that when different sectors come together with a shared goal, the results can be transformative. The One Health initiative isn’t just a concept—it’s a proven framework for achieving global disease prevention in a practical, impactful way.
Health Equity Worldwide: Bridging the Gap
Barriers to Health Equity Worldwide
Despite all the advancements in medicine and technology, achieving health equity worldwide remains one of the most pressing challenges of our time. At its core, health equity means that everyone has a fair opportunity to achieve their best possible health. But in reality, this ideal is far from being realized.
One of the biggest barriers is economic inequality. In many parts of the world, access to healthcare is heavily influenced by income. Those with financial resources can afford better treatments, while others struggle to access even basic services. This creates a cycle where poor health further limits economic opportunities, deepening the divide.
Geographical disparities also play a significant role. Rural and remote areas often lack healthcare facilities, trained professionals, and essential supplies. For people living in these regions, seeking medical care can involve long, costly journeys, making it less likely that they will receive timely treatment.
Cultural and social factors add another layer of complexity. Language barriers, discrimination, and lack of awareness can prevent individuals from accessing healthcare services. In some cases, traditional beliefs may conflict with modern medical practices, leading to hesitation or refusal to seek treatment.
Political and systemic issues further complicate the situation. Weak healthcare infrastructure, भ्रष्ट governance (corruption), and lack of policy support can hinder efforts to improve health outcomes. These challenges highlight the need for stronger public health collaboration and more inclusive policies.
Addressing these barriers requires a multifaceted approach that goes beyond healthcare alone. It involves tackling social determinants of health, such as education, housing, and employment, to create a more equitable environment for all.
Solutions to Promote Fair Healthcare Access
While the challenges are significant, there are also numerous strategies to promote health equity worldwide. One of the most effective is strengthening primary healthcare systems. By focusing on community-based care, countries can ensure that essential services are accessible to even the most underserved populations.
Investing in education is another powerful tool. When people are informed about their health and available services, they are more likely to seek care and make informed decisions. Health literacy plays a crucial role in bridging gaps and empowering individuals.
Technology can also be a game-changer. Telemedicine and mobile health platforms can bring healthcare services to remote areas, reducing geographical barriers. These innovations align with the broader goals of the global wellness movement, which emphasizes accessibility and inclusivity.
Policy reforms are equally important. Governments need to prioritize healthcare funding, implement equitable policies, and ensure accountability. International organizations can support these efforts by providing resources, expertise, and guidance.
Community engagement is perhaps the most critical factor. When local communities are involved in designing and implementing health programs, the solutions are more likely to be effective and sustainable. This approach fosters trust and ensures that interventions are culturally appropriate.
Achieving health equity worldwide is not an overnight process, but with consistent effort and collaboration, meaningful progress is possible. It’s about creating a world where health is a right, not a privilege.
Pandemic Preparedness Strategies for a Safer Tomorrow
Lessons Learned from Recent Global Pandemics
If recent history has taught us anything, it’s that pandemics can reshape the world in ways we never imagined. From healthcare systems to economies and daily life, the impact is far-reaching. That’s why understanding and improving pandemic preparedness strategies has become a global priority.
One of the most important lessons is the value of early action. Delays in recognizing and responding to outbreaks can lead to rapid spread, overwhelming healthcare systems. Countries that acted quickly—implementing testing, tracing, and isolation measures—were generally more successful in controlling the spread.
Another key takeaway is the importance of communication. Clear, consistent messaging helps build public trust and ensures that people follow guidelines. Misinformation, on the other hand, can undermine efforts and create confusion.
Supply chain resilience also emerged as a critical factor. Shortages of medical supplies, such as masks and ventilators, highlighted the need for better planning and coordination. Strengthening supply chains is essential for effective pandemic preparedness strategies.
The role of technology cannot be overlooked. From vaccine development to data tracking, technological innovations played a crucial role in managing the crisis. These advancements demonstrate the potential of healthcare innovation science in addressing global challenges.
Strengthening Pandemic Preparedness Strategies Globally
Building stronger pandemic preparedness strategies requires a proactive and collaborative approach. One of the first steps is investing in surveillance systems that can detect outbreaks early. These systems should integrate data from human, animal, and environmental sources, aligning with the principles of the One Health initiative.
Capacity building is another crucial aspect. Healthcare systems need to be equipped with the resources, infrastructure, and trained personnel required to handle large-scale health emergencies. This includes expanding hospital capacity, improving laboratory capabilities, and ensuring access to essential supplies.
International cooperation is also vital. Pandemics are global by nature, and no country can tackle them alone. Sharing information, resources, and best practices can significantly enhance global response efforts.
Research and development should be prioritized as well. Investing in vaccines, treatments, and diagnostic tools can accelerate responses to emerging threats. Public-private partnerships can play a key role in driving innovation and ensuring accessibility.
Finally, community involvement is essential. Public awareness and participation can make or break response efforts. Educating people about preventive measures and encouraging responsible behavior can significantly reduce the spread of diseases.
By strengthening these strategies, the world can move toward a future where pandemics are not just managed but effectively prevented.
Environmental Health Impact on Global Wellness Movement
Climate Change and Its Health Implications
If you’ve ever wondered how deeply the environment affects your daily life, just look at the growing momentum of the global wellness movement. It’s no longer just about fitness routines or healthy eating—it’s about understanding the broader environmental health impact on our physical and mental well-being. And at the center of this conversation sits climate change, quietly but powerfully reshaping global health patterns.
Rising global temperatures are not just numbers on a chart—they translate into real-world health risks. Heatwaves are becoming more frequent and intense, leading to dehydration, heatstroke, and even cardiovascular complications. Vulnerable populations, such as the elderly and children, are particularly at risk. But it doesn’t stop there. Warmer climates also create ideal conditions for disease-carrying vectors like mosquitoes, increasing the spread of illnesses such as dengue and malaria.
Air quality is another major concern. Increased pollution levels contribute to respiratory diseases, including asthma and chronic obstructive pulmonary disease (COPD). According to global health estimates, millions of premature deaths each year are linked to air pollution alone. That’s a staggering reminder of how closely environmental health impact is tied to human survival.
Water scarcity and contamination further complicate the picture. Climate change disrupts water cycles, leading to droughts in some regions and flooding in others. Both extremes can compromise water quality, increasing the risk of waterborne diseases. This directly affects communities and places additional strain on already stretched sustainable health systems.
What makes this issue even more urgent is its ripple effect. Environmental changes influence food security, mental health, and even migration patterns. The global wellness movement is increasingly recognizing that true wellness cannot exist without a healthy planet. It’s like trying to thrive in a house with a crumbling foundation—it simply doesn’t work.
Addressing these challenges requires collective action, from reducing carbon emissions to promoting eco-friendly practices. It’s not just about saving the planet; it’s about safeguarding our own health and future.
Environmental Health Impact on Daily Life
While climate change might sound like a large-scale issue, its effects are felt in the smallest details of our daily lives. The environmental health impact shows up in the air we breathe, the water we drink, and even the food on our plates. Once you start noticing these connections, it’s hard to ignore how deeply intertwined everything is.
Take urban living, for example. Many cities struggle with high levels of pollution, which can lead to chronic respiratory problems. People often adapt by staying indoors more, using air purifiers, or wearing masks. While these measures help, they also highlight a bigger issue—our environments are shaping our lifestyles in ways we didn’t anticipate.
Food quality is another area where environmental factors play a crucial role. Soil degradation, pesticide use, and climate variability all influence the nutritional value and safety of food. This directly affects human health, making human animal environmental health an essential consideration in agriculture and food systems.
Mental health is also impacted by environmental conditions. Exposure to green spaces has been shown to reduce stress and improve overall well-being. On the flip side, living in polluted or overcrowded environments can contribute to anxiety and depression. This connection is gaining recognition within the global wellness movement, which emphasizes holistic well-being.
Even everyday choices, like transportation and energy use, have health implications. Opting for cleaner alternatives not only benefits the environment but also reduces exposure to harmful pollutants. It’s a reminder that individual actions, when multiplied across populations, can drive meaningful change.
Understanding the environmental health impact on daily life encourages more mindful living. It shifts the focus from reactive healthcare to proactive wellness, aligning perfectly with the vision of “One World, One Health, One Science.”
Zoonotic Disease Control and Healthcare Innovation Science
Preventing Future Outbreaks Through Zoonotic Disease Control
One of the most critical areas in modern healthcare is zoonotic disease control, especially as the world becomes more interconnected. Zoonotic diseases—those that jump from animals to humans—account for a significant portion of emerging infectious diseases. This makes them a major focus of the One Health initiative and a key pillar in global disease prevention efforts.
Preventing these diseases starts with understanding their origins. Many zoonotic outbreaks are linked to human activities such as deforestation, wildlife trade, and intensive farming. These practices disrupt natural ecosystems, bringing humans and animals into closer contact and increasing the likelihood of disease transmission. It’s a classic case of unintended consequences—when we alter nature, nature responds.
Surveillance is one of the most effective tools in zoonotic disease control. Monitoring animal populations for unusual patterns of illness can provide early warning signs of potential outbreaks. This requires collaboration between veterinarians, environmental scientists, and healthcare professionals, reinforcing the importance of an integrated healthcare approach.
Regulation also plays a crucial role. Implementing strict guidelines for wildlife trade, improving biosecurity in farms, and promoting ethical animal practices can significantly reduce risks. These measures not only protect human health but also contribute to animal welfare and environmental sustainability.
Public awareness is equally important. Educating communities about safe practices, such as proper food handling and avoiding contact with wild animals, can help prevent transmission. When people understand the risks, they are more likely to adopt behaviors that protect themselves and others.
Ultimately, zoonotic disease control is about prevention rather than cure. It’s about addressing the root causes and creating systems that minimize risks. By doing so, we can reduce the likelihood of future pandemics and build a safer, healthier world.
Advancements in Healthcare Innovation Science
If prevention is the goal, then healthcare innovation science is the engine driving progress. Over the past decade, technological advancements have transformed how we detect, treat, and prevent diseases. And as we look toward the future, these innovations are set to play an even bigger role in shaping global health.
One of the most exciting developments is the use of artificial intelligence in healthcare. AI can analyze vast amounts of data to identify patterns, predict outbreaks, and even assist in diagnosis. This capability is particularly valuable for pandemic preparedness strategies, where speed and accuracy are critical.
Another breakthrough is in vaccine technology. The rapid development of vaccines during recent global health crises demonstrated what’s possible when science and collaboration come together. New platforms, such as mRNA vaccines, are paving the way for faster and more effective responses to emerging diseases.
Telemedicine continues to expand, improving access to healthcare services worldwide. This is especially important for achieving health equity worldwide, as it allows people in remote or underserved areas to receive medical care without significant barriers.
Wearable technology is also gaining traction. Devices that monitor vital signs in real time can help detect health issues early and provide valuable data for healthcare providers. This aligns with the goals of the global wellness movement, which emphasizes proactive and personalized care.
Biotechnology and genomics are opening new frontiers as well. From personalized medicine to advanced diagnostic tools, these innovations are revolutionizing healthcare. They enable more precise treatments and better outcomes, making healthcare systems more efficient and effective.
The future of health lies at the intersection of science, technology, and collaboration. Healthcare innovation science is not just about new tools—it’s about creating smarter, more connected systems that prioritize prevention, equity, and sustainability.
One World, One Health, One Science in Action
World Health Day 2026 isn’t just another date on the calendar—it’s a powerful reminder that health is a shared responsibility. The themes of global health awareness 2026, integrated healthcare approach, and the One Health initiative all point toward a single truth: our well-being is deeply interconnected. Whether it’s human animal environmental health, public health collaboration, or sustainable health systems, every piece plays a role in shaping a healthier future.
The journey ahead requires commitment, innovation, and cooperation. From strengthening pandemic preparedness strategies to addressing environmental health impact and advancing zoonotic disease control, the path forward is both challenging and full of opportunity. The global wellness movement continues to grow, encouraging individuals and communities to take proactive steps toward better health.
At its core, the vision of “One World, One Health, One Science” is about unity. It’s about breaking down barriers, sharing knowledge, and working together to create solutions that benefit everyone. When we embrace this mindset, we move closer to achieving health equity worldwide and ensuring a safer, healthier future for generations to come.
FAQs
1. What is the theme of World Health Day 2026?
The theme of World Health Day 2026 is “One World, One Health, One Science,” emphasizing the interconnectedness of human, animal, and environmental health.
2. Why is the One Health initiative important?
The One Health initiative is crucial because it promotes collaboration across multiple sectors to prevent diseases, improve health outcomes, and address global health challenges holistically.
3. How does environmental health impact human well-being?
The environmental health impact affects air quality, water safety, food systems, and climate conditions, all of which directly influence physical and mental health.
4. What are zoonotic diseases and why are they significant?
Zoonotic diseases are infections that spread from animals to humans. They are significant because they account for many emerging health threats and require coordinated prevention strategies.
5. How can individuals contribute to global health awareness 2026?
Individuals can support global health awareness 2026 by staying informed, practicing healthy behaviors, supporting sustainable practices, and participating in community health initiatives.


Leave a Reply