History and Significance of World IBS Day
Origins of World IBS Day
World IBS Day, observed every year on April 19, has gradually evolved from a niche awareness initiative into a globally recognized health observance. It was first established by healthcare professionals and advocacy groups who noticed a glaring gap—millions of people were silently suffering from Irritable Bowel Syndrome (IBS) without proper diagnosis, support, or even understanding. Unlike more visible health conditions, IBS often hides behind closed doors, masked by embarrassment and stigma, which makes awareness efforts even more crucial.
The early campaigns for World IBS Day were modest, mostly limited to small community events and online discussions. However, as digital platforms expanded, so did the reach of this awareness day. By the mid-2020s, global participation surged, with healthcare professionals, nutritionists, and patients sharing personal experiences, research findings, and management strategies. This collective effort has transformed World IBS Day into a powerful movement that amplifies voices that were once overlooked.

In 2026, the significance of this day feels even stronger. With increasing research into gut health and the microbiome, IBS is no longer dismissed as “just a stomach issue.” It is now understood as a complex condition involving the gut-brain axis, making awareness more critical than ever. The day serves not only as a reminder but also as a call to action—to improve diagnosis rates, reduce stigma, and encourage open conversations about digestive health.
Why Awareness Matters More Than Ever in 2026
In today’s fast-paced world, digestive health often takes a backseat until something goes wrong. IBS affects an estimated 10–15% of the global population, yet a significant number remain undiagnosed or misdiagnosed. That’s where World IBS Day 2026 steps in—it shines a spotlight on a condition that is both common and misunderstood.
Awareness plays a transformative role. When people understand IBS, they are more likely to seek help early rather than brushing off symptoms as temporary discomfort. It also encourages healthcare systems to prioritize research and develop better diagnostic tools. In 2026, discussions around IBS are no longer confined to clinics; they’re happening on social media, in workplaces, and even in schools, breaking down long-standing taboos.
There’s also a human side to this awareness. Living with IBS can be isolating. People often cancel plans, avoid travel, or feel anxious in social situations due to unpredictable symptoms. By raising awareness, World IBS Day fosters empathy and understanding, making it easier for individuals to share their experiences without fear of judgment.
What is IBS?
Understanding Irritable Bowel Syndrome
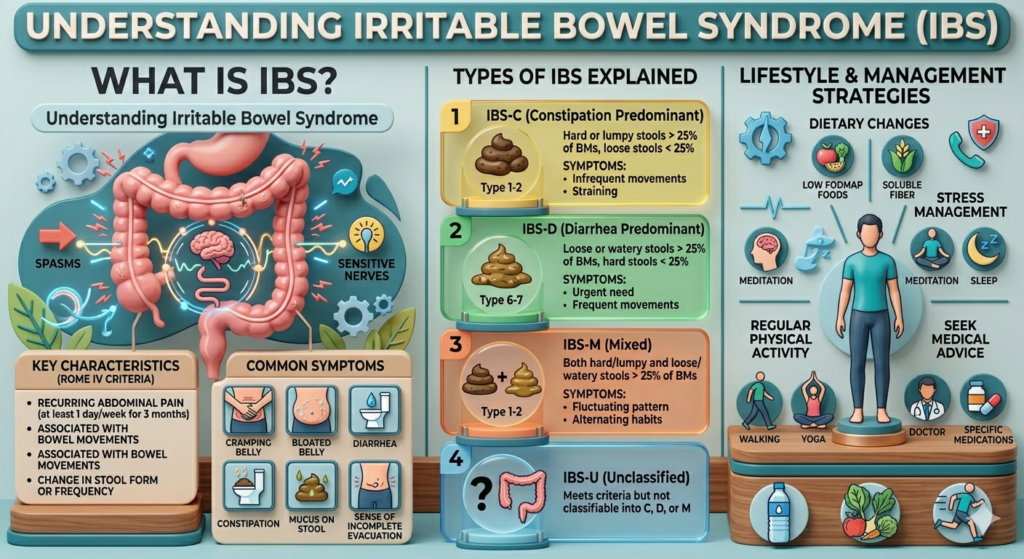
At its core, Irritable Bowel Syndrome (IBS) is a functional gastrointestinal disorder, meaning it affects how the digestive system works rather than causing visible damage. Think of it like a software glitch rather than a hardware failure—the system is intact, but the signals aren’t functioning smoothly. This distinction is important because it explains why IBS can be difficult to diagnose through traditional tests.
IBS primarily affects the large intestine and is characterized by a combination of symptoms such as abdominal pain, bloating, and changes in bowel habits. What makes IBS particularly challenging is its unpredictability. One day, everything might seem normal; the next, symptoms can flare up without warning. This inconsistency can disrupt daily life in ways that are hard for others to understand.
Another key aspect of IBS is its chronic nature. It’s not something that simply goes away after a few days. Instead, it tends to persist over time, with periods of remission and flare-ups. Despite this, IBS does not increase the risk of more serious conditions like cancer, which is an important reassurance for those newly diagnosed.
Types of IBS Explained
IBS is not a one-size-fits-all condition. It is generally categorized into different types based on the predominant bowel pattern. These include IBS with constipation (IBS-C), IBS with diarrhea (IBS-D), mixed IBS (IBS-M), and unclassified IBS. Each type presents its own challenges and requires tailored management strategies.
For example, someone with IBS-C may struggle with infrequent bowel movements and discomfort, while someone with IBS-D might deal with urgency and frequent trips to the bathroom. Mixed IBS can be particularly frustrating because symptoms alternate, making it harder to predict and manage.
Understanding these types is crucial because it influences treatment approaches. What works for one person might not work for another, highlighting the importance of personalized care in managing IBS effectively.
What Causes IBS?
Gut-Brain Connection and IBS
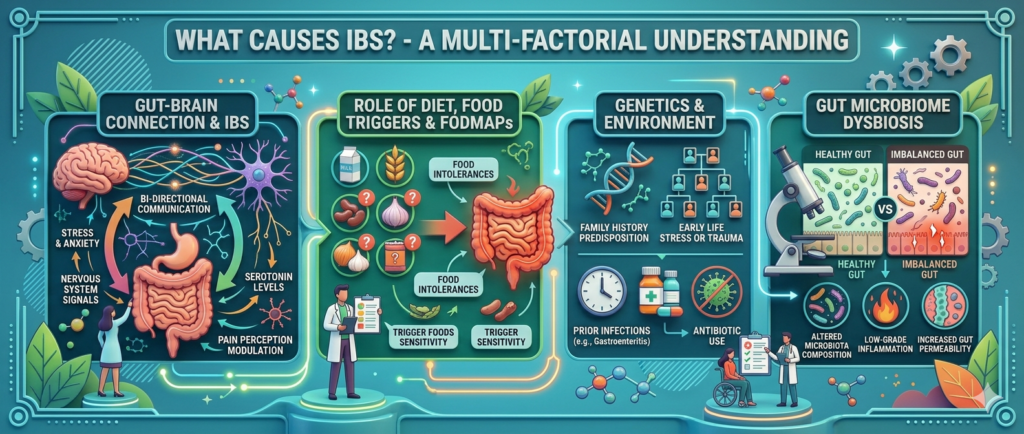
One of the most fascinating aspects of IBS is the gut-brain connection. The digestive system and the brain are in constant communication through a network known as the gut-brain axis. In people with IBS, this communication can become disrupted, leading to heightened sensitivity in the gut.
Imagine your gut as a highly sensitive microphone. In someone without IBS, it picks up normal signals at a moderate volume. In someone with IBS, that volume is turned up, making even minor digestive processes feel uncomfortable or painful. This heightened sensitivity is a hallmark of the condition.
Stress and emotions also play a significant role in this connection. Have you ever felt “butterflies” in your stomach before a big event? That’s the gut-brain axis in action. For people with IBS, this response can be amplified, triggering symptoms during stressful situations.
Role of Diet, Genetics, and Microbiome
While the gut-brain connection is central, other factors also contribute to IBS. Diet is one of the most influential. Certain foods, such as those high in fermentable carbohydrates, can trigger symptoms by causing gas and bloating. These are often referred to as FODMAPs, and managing their intake can make a significant difference.
Genetics may also play a role. If IBS runs in your family, you might be more likely to develop it. However, genetics alone do not determine the condition—it’s usually a combination of factors.
The gut microbiome, which consists of trillions of bacteria living in the digestive tract, is another key player. An imbalance in these bacteria can affect digestion and contribute to IBS symptoms. Ongoing research in 2026 continues to explore how modifying the microbiome could lead to more effective treatments.
What are the Symptoms of IBS?
Common Symptoms People Experience
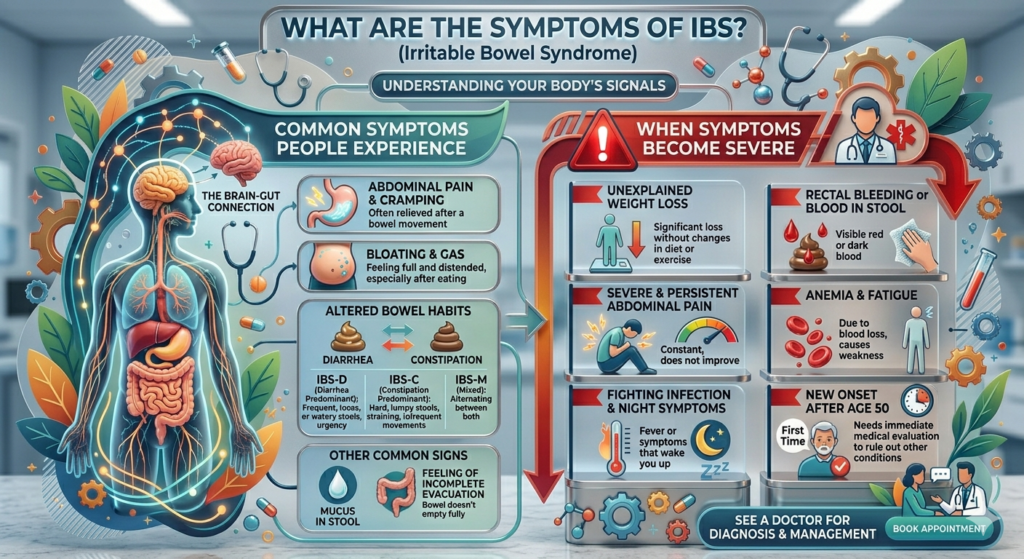
When it comes to Irritable Bowel Syndrome (IBS), the symptoms can feel like an unpredictable rollercoaster. One moment, everything seems fine, and the next, discomfort takes over your day. The most common symptoms include abdominal pain, bloating, gas, and noticeable changes in bowel habits such as diarrhea, constipation, or a mix of both. These symptoms aren’t just occasional inconveniences—they can persist for weeks, months, or even years, often appearing in cycles that make them difficult to anticipate.
Abdominal pain is often described as cramping and is usually relieved after a bowel movement. This detail might seem small, but it’s actually one of the key indicators doctors use when identifying IBS. Bloating, on the other hand, can make you feel like your stomach is stretched or swollen, even if you haven’t eaten much. It’s not uncommon for people with IBS to say they feel “full” or uncomfortable after normal-sized meals.
Another hallmark of IBS is the inconsistency in bowel movements. Some individuals may experience frequent diarrhea, while others struggle with constipation that feels stubborn and persistent. Then there are those who experience both, alternating between extremes. This variability is what makes IBS particularly frustrating—it doesn’t follow a predictable pattern.
Beyond the physical symptoms, there’s also an emotional layer. The constant need to locate a restroom, the fear of sudden flare-ups, and the embarrassment associated with digestive issues can weigh heavily on a person’s mental well-being. Over time, this can lead to anxiety or even avoidance of social situations, making IBS not just a physical condition but a lifestyle challenge.
When Symptoms Become Severe
While many people manage mild to moderate IBS symptoms, there are times when symptoms escalate and significantly impact daily life. Severe IBS can mean intense abdominal pain that disrupts sleep, frequent and urgent bowel movements that interfere with work or travel, or prolonged constipation that leads to additional complications like hemorrhoids.
One of the biggest concerns with severe symptoms is the overlap with other gastrointestinal conditions. For instance, sudden weight loss, blood in stool, or persistent pain that doesn’t improve should never be ignored. These signs may indicate something more serious and require immediate medical attention. IBS itself does not cause these alarming symptoms, so their presence is a red flag that needs further evaluation.
Severe IBS can also take a toll on nutrition. People may start avoiding certain foods out of fear of triggering symptoms, which can lead to an unbalanced diet. Over time, this can affect energy levels, immune function, and overall health. It becomes a delicate balancing act—trying to manage symptoms while still maintaining proper nutrition.
The emotional impact intensifies as well. Living with severe IBS often means planning your day around your symptoms, which can feel limiting and exhausting. However, recognizing when symptoms are severe is the first step toward seeking more advanced care and exploring targeted treatment options.
How is IBS Managed?
Personalized Treatment Approaches
Managing IBS isn’t about finding a one-size-fits-all solution—it’s more like assembling a personalized toolkit. What works wonders for one person might do very little for another. That’s why modern IBS management focuses on tailoring strategies to each individual’s symptoms, triggers, and lifestyle.
The first step usually involves identifying patterns. Keeping a food and symptom diary can reveal connections that aren’t immediately obvious. For example, you might notice that certain meals trigger bloating or that stress at work coincides with flare-ups. These insights become the foundation for building an effective management plan.
Healthcare professionals often take a holistic approach, combining dietary changes, lifestyle adjustments, and sometimes medication. This multi-layered strategy acknowledges that IBS is not just a digestive issue—it’s influenced by mental health, daily habits, and even sleep patterns.
Another important aspect of IBS management is patience. Unlike conditions where a single treatment provides immediate relief, IBS often requires trial and error. It may take time to find the right combination of strategies that works for you. This process can feel frustrating, but it’s also empowering because it puts you in control of your health journey.
Support systems also play a crucial role. Whether it’s a healthcare provider, a nutritionist, or even an online community, having someone to guide and encourage you can make a significant difference. Managing IBS is not just about reducing symptoms—it’s about improving quality of life.
Dietary Adjustments
Foods to Avoid and Include
Diet is one of the most powerful tools in managing IBS, but it can also be one of the most confusing. With so much conflicting information out there, it’s easy to feel overwhelmed. The key is to focus on understanding how your body reacts to different foods rather than following rigid rules.
One widely recognized approach is the low-FODMAP diet, which involves reducing foods that are known to ferment in the gut and cause gas and bloating. These include certain fruits, vegetables, dairy products, and grains. While this might sound restrictive, it’s usually implemented in phases—elimination, reintroduction, and personalization—so you can identify specific triggers without unnecessarily limiting your diet.
At the same time, it’s important to include foods that support digestive health. Fiber, for instance, plays a crucial role, but not all fiber is created equal. Soluble fiber, found in foods like oats and bananas, is generally better tolerated than insoluble fiber, which can sometimes worsen symptoms.
Hydration is another often-overlooked factor. Drinking enough water helps regulate digestion and can be particularly beneficial for those with constipation-predominant IBS. On the flip side, excessive caffeine or carbonated drinks may aggravate symptoms in some individuals.
Think of your diet as a balancing act rather than a strict set of dos and don’ts. The goal is to create a sustainable eating pattern that minimizes discomfort while still allowing you to enjoy your meals. Over time, these adjustments can lead to noticeable improvements in symptom control.
Lifestyle Modifications
Exercise and Daily Habits
Lifestyle choices have a profound impact on IBS, often in ways that aren’t immediately obvious. Regular physical activity, for example, does more than just keep you fit—it helps regulate bowel movements, reduce stress, and improve overall digestion. Even something as simple as a daily walk can make a noticeable difference.
Consistency is key when it comes to daily habits. Eating meals at regular times, getting enough sleep, and maintaining a routine can help stabilize your digestive system. Your gut thrives on predictability, so irregular schedules can sometimes trigger symptoms.
Sleep, in particular, deserves special attention. Poor sleep quality can exacerbate IBS symptoms, creating a cycle that’s hard to break. Prioritizing restful sleep by maintaining a consistent bedtime and minimizing screen time before bed can support both your mental and digestive health.
Another important habit is mindful eating. Rushing through meals or eating while distracted can lead to overeating or swallowing excess air, both of which can worsen IBS symptoms. Taking the time to chew thoroughly and savor your food can have surprisingly positive effects.
These lifestyle modifications might seem small on their own, but together, they create a foundation for better digestive health. It’s about building habits that support your body rather than working against it.
Stress Management
Mental Health and IBS Connection
The connection between stress and IBS is so strong that it’s often described as a two-way street. Stress can trigger IBS symptoms, and those symptoms, in turn, can increase stress. Breaking this cycle is a crucial part of managing the condition effectively.
Techniques such as mindfulness, meditation, and deep breathing exercises can help calm the nervous system and reduce the intensity of symptoms. These practices don’t require hours of commitment—even a few minutes a day can make a difference over time.
Cognitive behavioral strategies are also gaining attention for their effectiveness in managing IBS. By changing the way you respond to stress and symptoms, you can reduce their impact on your daily life. It’s not about eliminating stress entirely—that’s unrealistic—but about learning how to handle it more effectively.
Engaging in activities you enjoy, whether it’s reading, gardening, or spending time with loved ones, can also act as a natural stress reliever. These moments of relaxation are not just enjoyable—they’re therapeutic.
Understanding the mental health aspect of IBS is empowering. It shifts the focus from simply treating symptoms to addressing the underlying factors that contribute to them.
Medications and Supplements
Common Treatments Available
While lifestyle and dietary changes form the foundation of IBS management, medications and supplements can provide additional support when needed. These treatments are often tailored to the specific type of IBS and the severity of symptoms.
For example, individuals with IBS-D may benefit from medications that slow down bowel movements, while those with IBS-C might require treatments that promote regularity. Antispasmodics are commonly used to relieve abdominal pain and cramping by relaxing the muscles of the gut.
Supplements such as probiotics have also gained popularity. These aim to restore balance in the gut microbiome, potentially reducing symptoms like bloating and gas. However, their effectiveness can vary from person to person, so it’s important to approach them with realistic expectations.
It’s worth noting that medication is not a standalone solution. It works best when combined with other management strategies. Consulting a healthcare professional is essential to ensure that treatments are both safe and appropriate for your specific situation.
Challenges in IBS Diagnosis and Treatment

Misdiagnosis and Stigma
Despite its prevalence, IBS remains one of the most misunderstood digestive conditions. One of the biggest challenges is diagnosis. Since IBS does not cause visible damage to the digestive tract, it is often diagnosed based on symptoms rather than definitive tests. This can lead to delays, misdiagnoses, or even dismissal of symptoms.
Stigma adds another layer of complexity. Digestive issues are often considered embarrassing, which discourages people from seeking help or discussing their experiences openly. This silence can make individuals feel isolated, as if they are dealing with the condition alone.
There’s also the challenge of variability. IBS symptoms differ widely from person to person, making it difficult to develop standardized treatments. What works for one individual may not work for another, leading to frustration and trial-and-error approaches.
Addressing these challenges requires a combination of education, awareness, and empathy. As conversations around IBS become more open, the hope is that these barriers will gradually diminish.
Get Involved in World IBS Day 2026
Ways to Spread Awareness and Support
World IBS Day 2026 is more than just a date on the calendar—it’s an opportunity to make a real impact. Getting involved doesn’t require grand gestures; even small actions can contribute to a larger movement.
Sharing information on social media, participating in local events, or simply starting a conversation about IBS can help break the stigma. Education is one of the most powerful tools we have, and spreading accurate information can make a difference in how the condition is perceived.
Supporting someone with IBS is another meaningful way to get involved. Sometimes, understanding and empathy are more valuable than any medical treatment. Listening without judgment and being accommodating can go a long way in improving someone’s quality of life.
World IBS Day is also a reminder to prioritize your own health. If you’ve been experiencing symptoms but haven’t sought help, this could be the perfect time to take that step.
Conclusion
World IBS Day 2026 serves as a powerful reminder that Irritable Bowel Syndrome is real, common, and deserving of attention. From understanding its causes and symptoms to exploring effective management strategies, awareness is the first step toward change. As conversations continue to grow, so does the hope for better diagnosis, improved treatments, and a more compassionate understanding of those living with IBS.
FAQs
- What is World IBS Day 2026?
World IBS Day 2026 is an annual awareness event observed on April 19 to educate people about Irritable Bowel Syndrome and support those affected. - What are the main symptoms of IBS?
Common symptoms include abdominal pain, bloating, gas, diarrhea, constipation, or a combination of both. - Can IBS be cured permanently?
There is currently no permanent cure, but symptoms can be effectively managed through diet, lifestyle changes, and medical treatment. - What foods should be avoided in IBS?
Foods high in FODMAPs, caffeine, and processed items may trigger symptoms, though triggers vary by individual. - How can I participate in World IBS Day 2026?
You can spread awareness, support individuals with IBS, share educational content, and engage in community activities.


Leave a Reply