Understanding World Haemophilia Day and Its Global Importance
World Haemophilia Day is more than just a date on the calendar—it’s a powerful reminder of how awareness, education, and timely action can literally save lives. Observed every year on April 17, this day shines a spotlight on genetic bleeding disorders like haemophilia, encouraging individuals, families, and healthcare systems to take proactive steps toward better diagnosis and treatment. The significance of this day has grown over time, especially as more people begin to understand the silent yet dangerous nature of blood clotting disorders.
What makes World Haemophilia Day particularly important is its focus on bridging the knowledge gap. Many people still don’t recognize the early warning signs of haemophilia, leading to delayed diagnosis and preventable complications. Imagine living with a condition where even a small injury could lead to prolonged bleeding, yet not knowing the reason behind it. That’s the reality for countless individuals around the world who remain undiagnosed.
Globally, millions are affected by haemophilia and other bleeding disorders, yet access to proper care varies dramatically. In some regions, early diagnosis is standard practice, while in others, people may go years without understanding their condition. This disparity highlights why awareness campaigns tied to this day are essential. They encourage early screening, promote education, and foster conversations that can lead to life-saving interventions.
By emphasizing the importance of early diagnosis, World Haemophilia Day plays a crucial role in reducing complications, improving quality of life, and ensuring that individuals receive the care they need before severe symptoms arise. It’s not just about awareness—it’s about action, prevention, and hope for a healthier future.

Why Haemophilia Awareness Matters Today
Awareness is the first step toward prevention and effective management, and when it comes to haemophilia, it can make the difference between life and death. Despite medical advancements, haemophilia awareness remains surprisingly low in many parts of the world. This lack of awareness often leads to late diagnoses, which can result in irreversible joint damage, internal bleeding, and even fatal complications.
Think about it—how often do people consider excessive bruising or prolonged bleeding as a sign of a serious condition? Most dismiss it as something minor. That’s exactly why spreading awareness is so critical. By educating communities about haemophilia symptoms early detection, more individuals can recognize warning signs and seek medical help sooner rather than later.
Another reason awareness matters is the stigma associated with genetic conditions. In some cultures, families may hesitate to discuss or investigate hereditary disorders, fearing social consequences. This silence only worsens the situation, allowing the condition to go unnoticed across generations. Open conversations, fueled by awareness campaigns, can break this cycle and encourage proactive healthcare decisions.
Healthcare professionals also benefit from increased awareness. When doctors and nurses are trained to identify early symptoms, they can recommend appropriate haemophilia screening and diagnosis methods quickly. This leads to faster intervention and better outcomes for patients.
Ultimately, awareness transforms lives. It empowers individuals with knowledge, reduces fear, and promotes timely action. In the context of haemophilia, it ensures that fewer people suffer unnecessarily and more receive the care they deserve.
Global Impact of Genetic Bleeding Disorders
The global burden of genetic bleeding disorders is often underestimated, yet its impact is far-reaching and profound. Haemophilia, in particular, affects approximately 1 in 10,000 births worldwide, with thousands of cases still undiagnosed. These numbers only scratch the surface, as many individuals in low-resource regions lack access to proper testing and medical care.
One of the most striking aspects of this condition is its uneven distribution of healthcare resources. In developed countries, individuals with haemophilia often live near-normal lives due to early diagnosis and advanced treatment options. However, in developing regions, the story is drastically different. Limited access to diagnostic tools and treatment means that many people face severe complications or even premature death.
The economic impact is another critical factor. Managing haemophilia requires ongoing care, including clotting factor replacement therapy and regular monitoring. Without early diagnosis, the costs can skyrocket due to emergency treatments, hospitalizations, and long-term disabilities. This creates a significant financial burden not only for families but also for healthcare systems.
Beyond the numbers, the human impact is deeply personal. Children may grow up unable to participate in normal activities, adults may struggle with chronic pain, and families often live in constant fear of unexpected bleeding episodes. These challenges highlight the urgent need for improved haemophilia treatment awareness and accessible care worldwide.
Addressing the global impact of haemophilia requires a coordinated effort involving education, policy changes, and community support. By prioritizing early diagnosis and raising awareness, we can reduce disparities and ensure that everyone, regardless of location, has a chance at a healthier life.
What Is Haemophilia? A Deep Dive Into This Blood Clotting Disorder

Haemophilia is a rare but serious blood clotting disorder that prevents the blood from clotting properly. This condition occurs due to the absence or deficiency of specific clotting factors—proteins in the blood that help stop bleeding. Without these factors, even minor injuries can lead to prolonged bleeding, while internal bleeding can occur without any obvious cause.
To understand haemophilia, imagine your body as a well-organized emergency response system. When a blood vessel is damaged, clotting factors rush to the scene to form a clot and stop the bleeding. In individuals with haemophilia, this response is delayed or incomplete, leaving the body vulnerable. This simple yet critical malfunction can have life-threatening consequences if not managed properly.
There are different levels of severity in haemophilia, ranging from mild to severe. People with mild haemophilia may only experience excessive bleeding during surgeries or injuries, while those with severe forms may have spontaneous bleeding episodes, particularly in joints and muscles. These repeated bleeding events can lead to chronic pain and long-term joint damage.
One of the most important aspects of managing haemophilia is understanding its genetic nature. Since it is an inherited condition, families with a history of haemophilia must be especially vigilant. Early identification through haemophilia screening and diagnosis can make a significant difference in outcomes.
The good news is that advancements in medical science have made it possible to manage haemophilia effectively. With proper care, individuals can lead active and fulfilling lives. However, this largely depends on timely diagnosis and awareness, reinforcing the critical role of early detection in saving lives.
Types of Haemophilia and Their Differences
Haemophilia is not a one-size-fits-all condition. It exists in different forms, each with its own characteristics and challenges. The two primary types are Haemophilia A and Haemophilia B, both of which are caused by deficiencies in different clotting factors. Understanding these differences is essential for accurate diagnosis and effective treatment.
Haemophilia A is the most common type, accounting for nearly 80% of all cases. It is caused by a deficiency in clotting factor VIII. On the other hand, Haemophilia B, sometimes referred to as Christmas disease, results from a deficiency in clotting factor IX. While both types share similar symptoms, their treatment approaches may vary slightly depending on the specific factor involved.
There is also a rare form known as Haemophilia C, which is less severe and often goes undiagnosed. Unlike the other types, it affects both men and women and is associated with a deficiency in factor XI. This variation highlights the complexity of genetic bleeding disorders and the need for comprehensive diagnostic methods.
Severity levels further differentiate haemophilia cases. Individuals with severe haemophilia have less than 1% of the normal clotting factor, leading to frequent spontaneous bleeding. Those with moderate or mild forms may experience symptoms only under certain conditions. This variability can sometimes make haemophilia symptoms early detection more challenging.
Recognizing the type and severity of haemophilia is crucial for tailoring treatment plans. It ensures that patients receive the right level of care and helps prevent complications. This is why early diagnosis haemophilia is not just beneficial—it’s essential for effective disease management.
Causes and Inheritance of Genetic Bleeding Disorders
When you dig deeper into haemophilia, the genetic story behind it is both fascinating and crucial for understanding why early diagnosis haemophilia matters so much. This isn’t a condition that appears randomly in most cases—it’s typically inherited, passed down through families via specific genes linked to the X chromosome. That’s why haemophilia is far more common in males, while females are often carriers who may or may not show symptoms themselves.
Picture the gene responsible for clotting factors as a tiny instruction manual inside your DNA. If that manual has missing or incorrect instructions, the body simply can’t produce enough clotting factor VIII or IX. As a result, the blood loses its ability to clot efficiently. What’s particularly important here is that families may carry this mutation for generations without fully realizing it, especially if symptoms are mild or overlooked.
In some cases, haemophilia can also occur due to spontaneous genetic mutations, meaning there’s no prior family history. This makes haemophilia screening and diagnosis even more critical, because relying solely on family medical history can sometimes be misleading. Without proper testing, individuals may go undiagnosed until a serious bleeding episode occurs.
Understanding inheritance patterns also plays a big role in bleeding disorder prevention. Genetic counseling can help families assess risks before having children, allowing them to make informed decisions. It also prepares parents to monitor potential haemophilia symptoms early detection in newborns, which can be life-saving.
The takeaway here is simple but powerful: knowing the cause isn’t just about science—it’s about preparedness. When families understand how haemophilia is inherited, they’re better equipped to act early, seek medical advice, and ensure proper care from the very beginning.
Recognizing Haemophilia Symptoms Early Detection Saves Lives
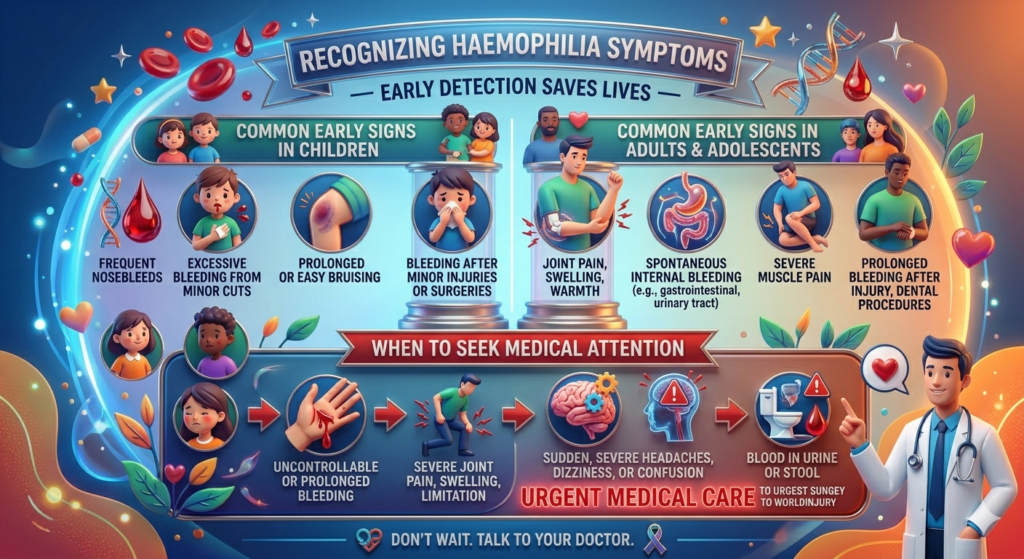
Spotting the early signs of haemophilia can feel like solving a puzzle, especially because symptoms aren’t always dramatic at first. Yet, recognizing these subtle clues is exactly what makes haemophilia symptoms early detection such a vital part of saving lives. The earlier the condition is identified, the sooner treatment can begin, reducing the risk of severe complications.
One of the most common early indicators is prolonged bleeding after minor injuries. For example, a small cut that takes unusually long to stop bleeding might seem harmless at first, but it could signal a deeper issue. Frequent nosebleeds, excessive bruising, and bleeding gums are other warning signs that shouldn’t be ignored. In infants, parents might notice unusual swelling or bruising once the child starts crawling or walking.
Internal bleeding is another serious concern. It often occurs in joints like knees, elbows, and ankles, causing pain, swelling, and limited movement. If left untreated, this can lead to permanent joint damage. This is why blood clotting disorder care must begin as early as possible.
What makes early detection challenging is that these symptoms can sometimes be mistaken for normal childhood injuries or minor health issues. That’s where awareness becomes critical. When parents and caregivers are educated about haemophilia awareness, they’re more likely to connect the dots and seek medical advice sooner.
Ultimately, early detection transforms outcomes. It turns a potentially life-threatening condition into a manageable one. By paying attention to the body’s signals and acting quickly, individuals can avoid unnecessary suffering and live healthier, more active lives.
Common Early Signs in Children and Adults
Understanding the early signs of haemophilia in both children and adults is like learning a new language—once you recognize the patterns, everything becomes clearer. In children, the signs often appear as soon as they become physically active. Frequent bruising, especially in unusual places, is one of the first red flags. Parents might also notice swelling in joints after minor bumps, which can indicate internal bleeding.
For infants, symptoms can be even more subtle. Prolonged bleeding after vaccinations or minor medical procedures is often one of the earliest indicators. Some babies may develop large bruises from simply being handled or learning to crawl. These signs might seem minor, but they are key to early diagnosis haemophilia.
In adults, especially those with mild haemophilia, symptoms may not become apparent until later in life. Excessive bleeding after dental work, surgeries, or injuries is a common sign. Women who are carriers may also experience heavy menstrual bleeding, which is often overlooked as a symptom of a genetic bleeding disorder.
The challenge lies in distinguishing these symptoms from everyday occurrences. After all, bruises and cuts are a normal part of life. But when they happen frequently or seem disproportionate to the injury, it’s worth paying attention. This is where haemophilia screening and diagnosis becomes essential.
Recognizing these early signs doesn’t require medical expertise—it requires awareness and attentiveness. By understanding what to look for, individuals and families can take the first step toward timely diagnosis and effective care.
When to Seek Medical Attention
Knowing when to seek medical attention can make all the difference in managing haemophilia effectively. The tricky part is that many early symptoms can appear mild or even routine, which often leads people to delay visiting a healthcare professional. But when it comes to early diagnosis haemophilia, hesitation can have serious consequences.
If someone experiences prolonged bleeding that doesn’t stop with basic first aid, it’s a clear sign that medical evaluation is needed. Similarly, frequent or unexplained bruising, especially in children, should never be ignored. Joint pain or swelling without a clear injury is another red flag that warrants immediate attention, as it could indicate internal bleeding.
For parents, it’s especially important to monitor infants and young children closely. Any unusual bleeding after routine procedures like vaccinations or minor cuts should prompt a visit to the doctor. Early intervention through proper haemophilia screening and diagnosis can prevent complications before they escalate.
Adults should also remain vigilant, particularly if they have a family history of genetic bleeding disorders. Unexpected bleeding during surgeries or dental procedures is often the first clue. Seeking medical advice at this stage can lead to timely diagnosis and appropriate treatment.
The bottom line is simple: when something feels off, don’t ignore it. Acting early not only helps confirm the condition but also opens the door to effective blood clotting disorder care. In many cases, that single decision to consult a doctor can be life-saving.
Importance of Early Diagnosis Haemophilia in Modern Healthcare

The importance of early diagnosis in haemophilia cannot be overstated—it’s the cornerstone of effective treatment and long-term health. In modern healthcare, early detection is what transforms haemophilia from a life-threatening condition into a manageable one. Without it, individuals face a higher risk of complications, including chronic pain, joint damage, and severe internal bleeding.
Think of early diagnosis as catching a small leak before it floods an entire house. When haemophilia is identified early, doctors can start preventive treatments that reduce the frequency and severity of bleeding episodes. This not only improves quality of life but also minimizes the need for emergency interventions.
One of the biggest advantages of early diagnosis haemophilia is the ability to implement prophylactic treatment. This involves regular infusions of clotting factors to prevent bleeding rather than reacting to it. Studies have shown that individuals who start preventive treatment early experience significantly fewer complications compared to those diagnosed later.
Early diagnosis also plays a crucial role in bleeding disorder prevention. It allows families to take necessary precautions, such as avoiding high-risk activities and ensuring prompt treatment for injuries. Additionally, it helps healthcare providers create personalized care plans tailored to the patient’s specific needs.
In today’s healthcare landscape, where precision medicine is becoming increasingly important, early diagnosis is more valuable than ever. It empowers patients, guides treatment decisions, and ultimately saves lives. The earlier haemophilia is detected, the better the outcomes—simple as that.
How Early Diagnosis Prevents Complications
Complications from haemophilia can be severe, but the good news is that many of them are preventable with early intervention. When haemophilia symptoms early detection leads to timely diagnosis, it allows healthcare providers to take proactive measures that significantly reduce risks.
One of the most common complications is joint damage caused by repeated internal bleeding. Over time, this can lead to chronic pain and limited mobility. However, with early diagnosis, preventive treatments can be started before significant damage occurs. This preserves joint health and allows individuals to maintain an active lifestyle.
Another major concern is life-threatening internal bleeding, particularly in vital organs like the brain. Early diagnosis ensures that patients and caregivers are aware of warning signs and can respond quickly in emergencies. This level of preparedness is a key aspect of effective blood clotting disorder care.
Infections and complications from untreated bleeding episodes are also reduced when haemophilia is diagnosed early. Regular monitoring and proper treatment minimize the chances of these issues, improving overall health outcomes.
Ultimately, early diagnosis acts as a protective shield. It doesn’t just treat the condition—it prevents the cascade of complications that can arise from delayed care. This is why raising haemophilia awareness and promoting early screening is so essential.
Life Expectancy Improvements With Early Care
Not too long ago, a diagnosis of haemophilia came with a heavy cloud of uncertainty, especially when it came to life expectancy. But today, thanks to early diagnosis haemophilia and advancements in treatment, that narrative has changed dramatically. People diagnosed early and managed properly can now live long, fulfilling lives that closely mirror those without the condition.
The key difference lies in timing. When haemophilia is identified early, healthcare providers can introduce preventive strategies before serious complications arise. This includes regular clotting factor replacement therapy, routine monitoring, and lifestyle adjustments that reduce the risk of injury. Over time, these measures significantly lower the chances of life-threatening bleeding episodes.
Statistics from global health organizations suggest that in countries with access to early diagnosis and modern care, life expectancy for individuals with haemophilia has increased by decades compared to previous generations. That’s a powerful testament to the importance of early diagnosis. It’s not just about managing symptoms—it’s about extending and improving life itself.
Another critical aspect is quality of life. Early care reduces hospital visits, minimizes chronic pain, and allows individuals to participate in everyday activities with confidence. Children can attend school without frequent interruptions, and adults can pursue careers and hobbies without constant fear of bleeding episodes.
The ripple effect extends to families as well. When haemophilia is diagnosed early, caregivers are better prepared, less anxious, and more capable of providing effective support. This creates a healthier, more stable environment for everyone involved.
In essence, early diagnosis doesn’t just add years to life—it adds life to those years. It transforms haemophilia from a limiting condition into one that can be managed with confidence and control.
Haemophilia Screening and Diagnosis Methods Explained
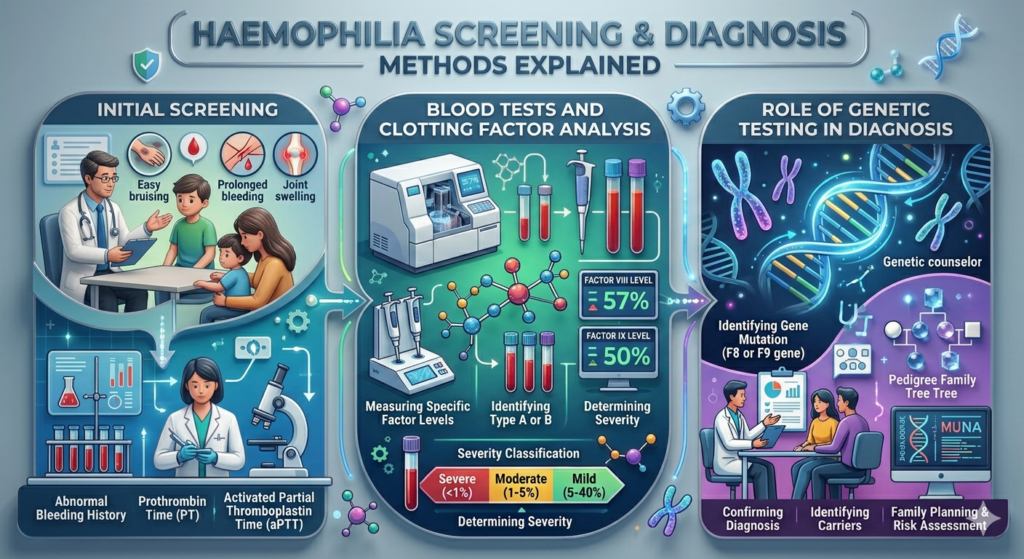
Understanding how haemophilia is identified is a crucial step in promoting haemophilia screening and diagnosis. The process isn’t as complicated as it might sound, but it does require awareness and timely action. Early screening is often the bridge between suspicion and confirmation, turning uncertainty into a clear path forward.
Diagnosis typically begins with a detailed medical history and physical examination. Doctors look for patterns—frequent bruising, prolonged bleeding, or a family history of genetic bleeding disorders. These clues help guide further testing and ensure that nothing is overlooked.
Laboratory tests are the backbone of diagnosis. Blood tests measure how long it takes for blood to clot and identify deficiencies in specific clotting factors. These tests are highly accurate and can determine not only the presence of haemophilia but also its severity. This information is essential for creating an effective treatment plan.
Early screening is especially important for newborns with a family history of haemophilia. In many cases, testing can be done shortly after birth, allowing for immediate intervention if needed. This proactive approach is a cornerstone of bleeding disorder prevention, as it reduces the risk of complications from the very beginning.
Another important aspect is accessibility. While advanced diagnostic tools are widely available in developed regions, there is still a need to expand access globally. Increasing awareness and improving healthcare infrastructure can ensure that more people benefit from early detection.
Ultimately, the goal of screening and diagnosis is simple: catch the condition early and act quickly. When this happens, the chances of living a healthy, normal life increase significantly.
Blood Tests and Clotting Factor Analysis
Blood tests are the frontline tools in identifying haemophilia, and they play a central role in haemophilia screening and diagnosis. These tests go beyond basic health checks—they dive deep into how well the blood performs its essential function of clotting.
The most common tests include clotting time assessments, such as the activated partial thromboplastin time (aPTT) test. If this test shows prolonged clotting, it raises a red flag that further investigation is needed. From there, specific clotting factor assays are conducted to measure the levels of factor VIII or IX in the blood.
Think of these tests as detectives uncovering clues. Each result adds a piece to the puzzle, helping doctors determine whether haemophilia is present and how severe it is. This level of precision is critical for planning appropriate blood clotting disorder care.
One of the advantages of these tests is their reliability. They provide clear, measurable results that leave little room for doubt. This is particularly important when diagnosing mild cases, where symptoms may not be obvious.
Regular monitoring through blood tests is also essential after diagnosis. It helps track the effectiveness of treatment and ensures that clotting factor levels remain within a safe range. This ongoing care is a vital part of haemophilia treatment awareness, as it empowers patients to stay in control of their condition.
In short, blood tests are more than just diagnostic tools—they are the foundation of effective haemophilia management.
Role of Genetic Testing in Diagnosis
Genetic testing has added a whole new dimension to haemophilia screening and diagnosis, making it possible to identify the condition even before symptoms appear. This is particularly valuable for families with a history of genetic bleeding disorders, as it provides clarity and direction for future planning.
Unlike standard blood tests, genetic testing looks directly at the DNA to identify mutations responsible for haemophilia. This can confirm a diagnosis, determine carrier status, and even predict the likelihood of passing the condition to future generations. It’s like having a roadmap that guides both medical and personal decisions.
For expectant parents, genetic testing can be life-changing. Prenatal testing allows doctors to identify whether a baby will have haemophilia, enabling early preparation and specialized care at birth. This level of foresight is a powerful tool in bleeding disorder prevention.
Another benefit is the ability to detect carriers, particularly among women who may not show symptoms. Knowing carrier status allows families to make informed decisions and seek appropriate medical guidance.
While genetic testing is highly effective, it also raises important ethical and emotional considerations. Counseling is often recommended to help individuals understand the results and their implications.
Overall, genetic testing represents a significant step forward in haemophilia care. It complements traditional diagnostic methods and reinforces the importance of early diagnosis, ensuring that no case goes unnoticed.
Haemophilia Treatment Awareness and Management Strategies
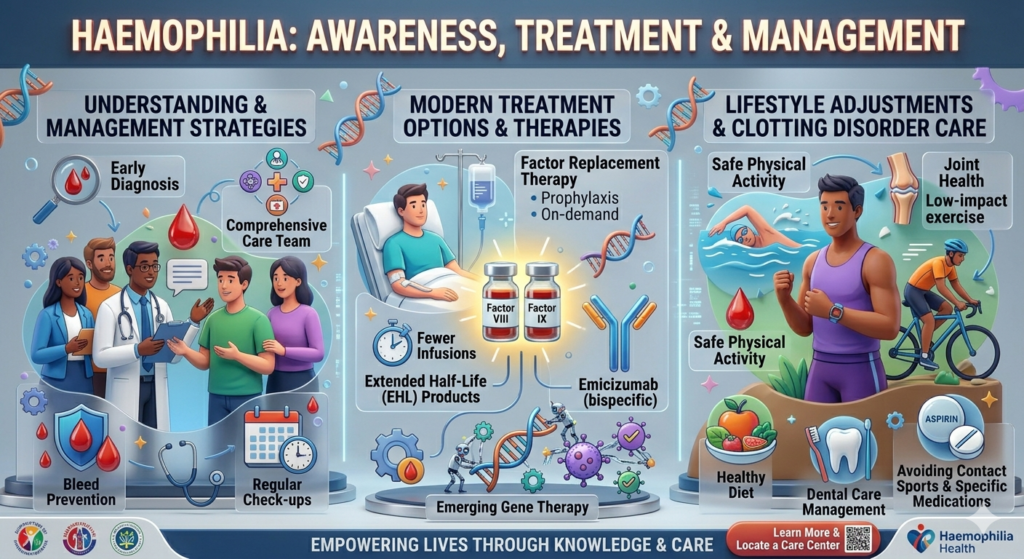
Raising haemophilia treatment awareness is just as important as diagnosing the condition itself. After all, knowing you have haemophilia is only the first step—the real challenge lies in managing it effectively. The good news is that modern medicine offers a range of treatment options that can significantly improve quality of life.
The cornerstone of treatment is clotting factor replacement therapy. This involves injecting the missing clotting factor into the bloodstream to help the blood clot normally. Depending on the severity, this can be done on-demand (during bleeding episodes) or as a preventive measure.
In recent years, newer therapies have emerged, including long-acting clotting factors and non-factor treatments. These innovations reduce the frequency of injections and provide more consistent protection against bleeding. This progress highlights the importance of staying informed and engaged in haemophilia treatment awareness.
Management also extends beyond medication. Lifestyle choices play a crucial role in blood clotting disorder care. Avoiding high-risk activities, maintaining a healthy weight, and engaging in safe physical exercises can all help reduce the risk of bleeding.
Education is another key component. Patients and caregivers must understand how to recognize symptoms, administer treatment, and respond to emergencies. This knowledge empowers them to take control of the condition rather than being controlled by it.
In essence, effective management is a combination of medical care, lifestyle adjustments, and continuous learning. When these elements come together, individuals with haemophilia can lead active, fulfilling lives.
Modern Treatment Options and Therapies
The landscape of haemophilia treatment has evolved dramatically, offering hope and flexibility that were once unimaginable. Today’s therapies are designed not just to treat bleeding episodes but to prevent them altogether, making early diagnosis haemophilia even more impactful.
Clotting factor concentrates remain the gold standard. These can be derived from plasma or produced using recombinant technology, ensuring safety and effectiveness. Long-acting versions have reduced the frequency of infusions, making treatment more convenient.
Non-factor therapies, such as monoclonal antibodies, have introduced a new way of managing haemophilia. These treatments mimic the function of missing clotting factors, providing continuous protection with fewer injections. This innovation has been a game-changer for many patients.
Gene therapy is another exciting development. Although still evolving, it aims to correct the underlying genetic defect, potentially offering a long-term or even permanent solution. This represents a major leap forward in haemophilia treatment awareness and future care.
Each treatment option comes with its own benefits and considerations, which is why personalized care plans are essential. With the right approach, individuals can manage their condition effectively and enjoy a higher quality of life.
Lifestyle Adjustments and Blood Clotting Disorder Care
Living with haemophilia requires thoughtful lifestyle choices, but it doesn’t mean giving up on an active and enjoyable life. In fact, proper blood clotting disorder care is all about finding balance—knowing what to avoid while embracing what’s safe and beneficial.
Physical activity is a great example. While high-impact sports may pose risks, low-impact exercises like swimming, walking, and cycling can strengthen muscles and protect joints. Strong muscles act like natural shields, reducing the likelihood of bleeding episodes.
Diet also plays a role. Maintaining a healthy weight reduces stress on joints, which is particularly important for individuals prone to internal bleeding. Good nutrition supports overall health and enhances the body’s ability to recover from injuries.
Another important aspect is injury prevention. Simple measures like wearing protective gear, childproofing the home, and practicing safe habits can go a long way in bleeding disorder prevention. These precautions may seem small, but they make a big difference over time.
Emotional well-being shouldn’t be overlooked either. Living with a chronic condition can be challenging, but support from family, friends, and healthcare professionals can make it more manageable. Education and awareness help reduce fear and build confidence.
Ultimately, lifestyle adjustments are about empowerment. They allow individuals with haemophilia to take control of their health and live life on their own terms.
Bleeding Disorder Prevention and Risk Reduction
When people hear the word “genetic,” they often assume there’s nothing they can do to prevent or reduce risks—but that’s not entirely true. While haemophilia itself may not always be preventable, bleeding disorder prevention focuses on minimizing complications, reducing risks, and improving long-term outcomes. This is where awareness, education, and early action come together in a powerful way.
The idea of prevention in haemophilia is less about stopping the condition from existing and more about controlling how it affects daily life. For instance, individuals diagnosed early can begin preventive treatments that significantly reduce bleeding episodes. This approach, often called prophylaxis, helps maintain healthy joints and prevents long-term damage. It’s like maintaining a car regularly instead of waiting for it to break down—consistent care keeps everything running smoothly.
Risk reduction also involves understanding triggers. Certain activities, medications, or even lifestyle habits can increase the likelihood of bleeding. Being aware of these factors allows individuals to make safer choices without feeling restricted. This is why haemophilia awareness plays such a crucial role—it equips people with the knowledge they need to protect themselves.
Another important aspect is community education. Schools, workplaces, and public spaces should be informed about haemophilia so they can respond appropriately in case of emergencies. Imagine a child with haemophilia feeling safe at school because teachers know how to handle a bleeding episode—that’s the kind of impact awareness can have.
Preventive strategies also extend to vaccinations and regular health check-ups. These measures help avoid complications that could worsen bleeding conditions. Combined with proper blood clotting disorder care, they create a strong foundation for a healthier life.
Ultimately, prevention isn’t about limitation—it’s about preparation. It’s about giving individuals the tools and confidence to live fully while managing their condition effectively.
Preventive Care for High-Risk Individuals
For individuals at high risk—especially those with a family history of haemophilia—preventive care becomes a lifeline. It’s not just about reacting to symptoms but staying one step ahead. This proactive mindset is at the heart of early diagnosis haemophilia and effective long-term management.
High-risk individuals often include newborns in affected families, carriers, and those who have shown mild symptoms in the past. For these groups, regular monitoring is essential. Routine blood tests and medical evaluations can detect changes early, allowing for timely intervention. This approach reduces the likelihood of severe bleeding episodes and long-term complications.
Preventive care also involves education. Families need to understand how haemophilia works, what symptoms to watch for, and how to respond in emergencies. This knowledge transforms fear into confidence, making it easier to handle challenges as they arise. It also reinforces the importance of early diagnosis, as recognizing symptoms quickly can lead to faster treatment.
Vaccination protocols may require special attention for high-risk individuals. Injections should be administered carefully to minimize bleeding, often with guidance from healthcare professionals. These small adjustments make a big difference in bleeding disorder prevention.
Another key element is creating a safe environment. For children, this might mean using protective gear during play or modifying certain activities. For adults, it could involve workplace adjustments or avoiding high-risk situations. These measures aren’t about restriction—they’re about smart, informed choices.
Preventive care is ultimately about control. It allows high-risk individuals to manage their condition proactively rather than reactively, leading to better health outcomes and a more confident approach to life.
Educating Families About Genetic Risks
Education is one of the most powerful tools in managing genetic bleeding disorders, especially when it comes to families. Understanding how haemophilia is inherited can feel overwhelming at first, but once the pieces fall into place, it becomes a source of empowerment rather than fear.
Families who are aware of their genetic risks can take proactive steps, such as seeking genetic counseling before planning children. This doesn’t mean avoiding parenthood—it means being prepared. Knowing the chances of passing on haemophilia allows families to explore options and make informed decisions.
Education also helps break down misconceptions. In many cases, haemophilia is misunderstood, leading to unnecessary stigma or fear. By spreading accurate information, families can create a supportive environment where individuals feel understood and accepted. This is a key aspect of haemophilia awareness.
Children growing up in informed families benefit immensely. They learn about their condition early, understand how to manage it, and develop a sense of responsibility for their health. This early exposure reinforces the value of haemophilia symptoms early detection, as they become more attuned to their bodies.
Support networks also play a role. Connecting with other families facing similar challenges can provide emotional support and practical advice. These communities often become a source of strength and encouragement.
In the end, education turns uncertainty into clarity. It equips families with the knowledge they need to navigate haemophilia confidently, ensuring better outcomes for future generations.
Challenges in Early Diagnosis Haemophilia Worldwide
Despite advancements in medicine, achieving early diagnosis haemophilia on a global scale remains a significant challenge. The gap between developed and developing regions is still wide, and many individuals continue to live without proper diagnosis or care. This disparity highlights the urgent need for improved awareness and healthcare access worldwide.
One of the biggest obstacles is limited access to diagnostic facilities. In many low-resource settings, basic blood tests required for haemophilia screening and diagnosis are not readily available. This means that even when symptoms are present, confirming the condition can be difficult or delayed.
Another challenge is lack of awareness among both the public and healthcare professionals. In some areas, haemophilia is still poorly understood, leading to misdiagnosis or underdiagnosis. Symptoms may be attributed to other conditions, delaying proper treatment and increasing the risk of complications.
Cultural factors can also play a role. In certain communities, discussing genetic conditions may be taboo, preventing families from seeking medical help. This silence can allow haemophilia to go unnoticed for generations.
Financial barriers further complicate the situation. Diagnostic tests and treatments can be expensive, making them inaccessible to many families. Without financial support or healthcare infrastructure, early diagnosis becomes a luxury rather than a standard practice.
Addressing these challenges requires a global effort. Governments, healthcare organizations, and communities must work together to improve access, raise awareness, and promote early screening. Only then can the benefits of early diagnosis reach everyone, regardless of where they live.
Barriers in Low-Resource Settings
In low-resource settings, the journey to diagnosis is often filled with obstacles that go beyond medical limitations. These barriers make early diagnosis haemophilia particularly difficult, leaving many individuals undiagnosed or diagnosed too late.
Healthcare infrastructure is a major issue. Clinics may lack the equipment needed for accurate haemophilia screening and diagnosis, and trained professionals may be scarce. This creates a situation where even basic testing becomes a challenge.
Transportation and accessibility also play a role. In rural areas, reaching a healthcare facility can require long travel times, discouraging families from seeking help. This delay can be critical, especially when dealing with a condition that requires timely intervention.
Education and awareness are equally important. Without proper knowledge of haemophilia symptoms early detection, families may not recognize the need for medical attention. This lack of awareness often leads to delayed diagnosis and increased complications.
Addressing these barriers requires innovative solutions, such as mobile clinics, telemedicine, and community outreach programs. These initiatives can bring healthcare closer to those in need, making early diagnosis more achievable.
Why Early Diagnosis Is the Key to Saving Lives
World Haemophilia Day serves as a powerful reminder that awareness and action go hand in hand. The journey from recognizing symptoms to receiving proper care begins with understanding the importance of early diagnosis. When haemophilia is detected early, it opens the door to effective treatment, better quality of life, and significantly improved outcomes.
From identifying haemophilia symptoms early detection to implementing preventive strategies, every step plays a role in saving lives. Early diagnosis doesn’t just benefit individuals—it strengthens families, communities, and healthcare systems as a whole.
As awareness continues to grow, so does the hope for a future where no one suffers due to delayed diagnosis. By prioritizing education, improving access to care, and encouraging proactive health decisions, we can make that future a reality.
FAQs
1. What is World Haemophilia Day and why is it important?
World Haemophilia Day is observed on April 17 to raise awareness about haemophilia and other genetic bleeding disorders. It highlights the need for early diagnosis, proper treatment, and global access to care.
2. What are the early symptoms of haemophilia?
Common symptoms include prolonged bleeding, frequent bruising, joint pain, and unexplained swelling. Recognizing these signs is crucial for haemophilia symptoms early detection.
3. How is haemophilia diagnosed?
Diagnosis involves blood tests to measure clotting time and factor levels, along with genetic testing. These methods are part of haemophilia screening and diagnosis.
4. Why is early diagnosis of haemophilia important?
The importance of early diagnosis lies in preventing complications, improving quality of life, and enabling timely treatment.
5. Can haemophilia be prevented?
While the condition itself may not always be preventable, bleeding disorder prevention focuses on reducing risks, managing symptoms, and improving outcomes through early care.


Leave a Reply